When Nurse Practitioners Step Forward
Keith Carlson, RN, BSN, NC-BC
January, 2017
Nurse practitioners have been in the news in early 2017, and for very good reason; the time for nurse practitioners (NPs) and advanced practice registered nurses (APRNs) to step forward has come, and the world is taking notice.
In defining NPs, the American Association of Nurse Practitioners (AANP) states the following on their website:
“Nurse Practitioners (NPs) have been providing primary, acute and specialty healthcare to patients of all ages and walks of life for nearly half a century. NPs assess patients, order and interpret diagnostic tests, make diagnoses, and initiate and manage treatment plans – including prescribing medications. They are the healthcare providers of choice for millions of patients.”
While nurse practitioners have historically worked under the supervision of physicians, a growing movement to grant NPs complete autonomy and a broader scope of practice has taken hold, and it appears that critical mass has been achieved vis-à-vis nurse practitioners’ 21st-century coming of age.
Growing Autonomy for NPs
At the time of this writing, the AANP reports that 21 states and the District of Columbia (highlighted in green in the map below) have granted full autonomy to nurse practitioners. In such non-restrictive practice environments, NPs enjoy the ability to assess, diagnose, and treat patients without physician oversight or supervision; this increases their ability to meet the needs of patients who might otherwise lack access to primary care.
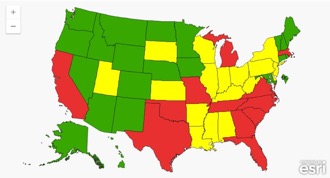
Image Source: AANP State Practice Environment, State Regulatory Map
With expanded access to primary care from nurse practitioners, patients who might otherwise seek treatment for minor complaints in the emergency room will instead have access to fully trained nurse practitioners who are able to meet the majority of primary care-related medical needs. When we relieve the unnecessary burden on emergency departments in regards to the provision of non-emergent care, we increase ER capacity and intelligently streamline the efficiency of healthcare delivery.
The highly influential Henry J. Kaiser Foundation makes this unequivocal statement in support of NPs on its website:
“Primary care NPs are significantly more likely than primary care physicians to practice in urban and rural areas, provide care in a wider range of community settings, and serve a high proportion of uninsured patients and other vulnerable populations. Studies show that NPs can manage 80-90% of care provided by primary care physicians. In addition, evidence from a substantial research literature shows that primary care outcomes, including disease-specific physiologic measures, improvement in pathological condition, reduction of symptoms, mortality, hospitalization and other utilization measures, and patient satisfaction, are comparable between patients served by NPs and patients served by physicians.”
By so ardently supporting the efficacy and accessibility of nurse practitioners, the Kaiser health policy think tank makes a strong argument for the ways in which NPs can be utilized to fill the widening gap in primary care, especially in relation to vulnerable populations in underserved locations around the United States.
The VA Steps In
News stories abound of veterans languishing without care despite their having sacrificed so much in service to their country. Politicians, veterans groups, and healthcare advocates similarly decry this reprehensible state of affairs, yet the reports of veterans without proper care continue to emerge.
As of January 13, 2017, nurse practitioners were granted complete autonomy of practice within the entirety of the Veterans Administration healthcare system. Even in states where NP and APRN practice is highly restricted by those states’ boards of nursing, nurse practitioners and advanced practice registered nurses working within the VA system now enjoy the unfettered ability to serve veterans who so clearly deserve such access to care.
Image Source: WPR News, Photographer: Connor Tarter (CC-BY-SA)
The Veterans Administration obviously understands the ways in which nurse practitioners can powerfully stem the tide of diminished access to care for veterans seeking support and treatment for a variety of health concerns. While the American Medical Association criticized the VA’s decision, the VA shows no signs of backing down from a decision that has already taken effect.
Echoes of Support for NPs
Many in the nursing community hypothesize that longitudinal data from the Veteran Administration’s records will echo the conclusions already drawn by the Henry J. Kaiser Foundation, as well as that of the equally influential Robert Wood Johnson Foundation, which has itself championed APRNs as an answer to the growing nationwide shortage of primary care physicians.
The American Association of Colleges of Nursing has tenaciously supported broader scope of practice for NPs and APRNs for years; the AACN is clear in its stance regarding the AMA’s opposition to APRN/NP autonomy:
“(The) AMA has no data to substantiate a charge of increased risk by advanced nurses who are practicing independently within their education and scope of practice. Evidence to date indicates that the quality of care by advanced practice nurses is at least equal to, and sometimes better than, comparable services by primary care physicians.
“Arguments in AMA's report are too little too late. The report stakes an exclusive claim to a field that organized medicine has largely abandoned. The AMA cannot justify restricting advanced nurses from serving as front-line, first points of contact for primary care, when medicine neither can produce enough future physicians to provide that care, nor has demonstrated a willingness so far to be on the front lines in sufficient numbers providing it.”
The arguments against NP autonomy continue, however the statistics certainly favor the effectiveness and safety of NP practice. APRNs themselves understand their scope of practice in the face of the same potential liability as physicians; it is therefore in nurse practitioners’ natural best interests to administer care within their acknowledged scope of practice in deference to patient safety and prudent regulatory adherence.
Nurse Practitioners Rise
As nurse practitioners become an increasingly accepted presence within mainstream healthcare delivery, Americans will continue to embrace them as purveyors of accessible, evidence-based, compassionate care.
The NP and nursing community is clear in its desire to fill the gaps, increase access, and provide the care that its members are trained to deliver across the lifespan. Nurse practitioners don’t want to perform open-heart surgery or forcibly push physicians out of their lucrative and deserving specialties. NPs understand their own scope of practice, and acknowledge the role that they can continue to play in the broader American healthcare system, especially in relation to the provision of primary care for patients in every decade of life.
Specially trained clinical nurse specialists (advanced practice nurses who generally serve in consulting and educational roles within the inpatient environment) can work alongside surgeons and other specialists in the hospital setting; however, they too have no desire to supersede doctors. Nursing is a collaborative profession, and it’s the cross-pollination of multidisciplinary care delivery that is one of the hallmarks of nursing practice.
The 21st century will see the continued ascendancy of nurse practitioners and APRNs into the mainstream; in short order, a significant number of Americans will have been seen by, or come into contact with, a nurse practitioner at some point in the course of their care.
From community health centers and VA clinics to freestanding NP primary care practices, nurse practitioners will no doubt change the face of primary care while also increasing accessibility. The NP revolution has begun.

Keith Carlson, RN, BSN, NC-BC
Keith Carlson is a holistic career coach for nurses, award-winning nurse blogger, writer, podcaster, speaker, author, and popular career columnist. He writes for his blog "Nurse Keith" and LPNtoBSNonline.org, and can also be found on Facebook, Twitter, LinkedIn, and Instagram.